Blog
December 4, 2025
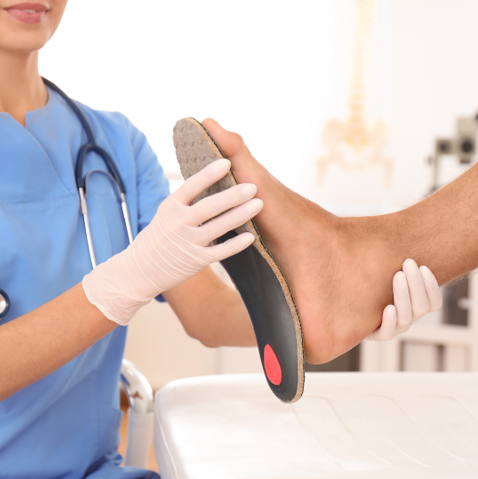
December is the season of giving, and there’s no better gift than comfort. If you’re looking for something meaningful, helpful, and long-lasting, custom orthotics are a great choice. They support the feet, improve balance, and make everyday activities easier and more comfortable. Why Orthotics Make a Great Gift Many people struggle with foot pain, tired feet, or discomfort when walking or standing. Custom orthotics can help by: Reducing foot, heel, and arch pain Providing better alignment and support Improving comfort during work, exercise, and daily routines Helping prevent future foot problems They are a thoughtful gift for anyone—especially those who stay on their feet all day, enjoy being active, or dealing with ongoing foot issues. How Our Team Can Help Our podiatry team offers: Custom Orthotic Fittings tailored to your foot shape and needs Foot Evaluations to identify pain points and pressure areas Supportive Shoe Recommendations for everyday comfort Ongoing Care for long-term foot health Give Comfort This Christmas If you’re searching for a gift that truly helps someone feel better, custom orthotics are a smart and meaningful choice. Contact our office to schedule an appointment or learn more about how orthotics can bring comfort all year long.